Theme: Emerging Technologies and treatment in Tumor & Cancer immunotherapy from vaccines to antibodies and cell therapies
Tumor & Cancer Immunology 2017
Track 1: Tumors
A Tumor is an abnormal growth of body tissue. Tumors can be cancerous (malignant) or noncancerous (benign). Tumors are of many types such as Carcinoid Tumor, Pituitary Tumor, and Tumor lysis syndrome. In general, tumors occur when cells divide and grow excessively in the body. Normally, the body controls cell growth and division. New cells are created to replace older ones or to perform new functions. Cells that are damaged or no longer needed die to make room for healthy replacements. If the balance of cell growth and death is disturbed, a Tumor may form. Problems with the body's immune system can lead to tumors. Carcinoid tumors are of neuroendocrine origin and derived from primitive stem cells in the gut wall, but they can be seen in other organs, including the lungs, mediastinum, thymus, liver, pancreas, bronchus, ovaries, prostate, and kidneys .Carcinoid tumors have high potential for metastasis.
Track 2: Brain Tumors
A primary brain Tumor is one that originates in the brain, and not all primary brain tumors are cancerous; benign tumors are not aggressive and normally do not spread to surrounding tissues, although they can be serious and even life threatening. Primary brain tumors emerge from the various cells that make up the brain and central nervous system and are named for the kind of cell in which they first form. The most common types of adult brain tumors are gliomas and astrocytic tumors. These tumors form from astrocytes and other types of glial cells, which are cells that help, keep nerves healthy. The second most common type of adult brain tumors are meningeal tumors. These form in the meninges, the thin layer of tissue that covers the brain and spinal cord.
Track 3: Tumor Immunology
The molecular classification of Tumor is actually arrangement analysis disguised as classification. In a typical gene expression array study, the researcher will look at a cluster of tumors of a specific type. Cluster analysis of the gene expression array values will help discrete the tumors into groups with common expression patterns. Some of these groupings will prove to have a detailed biologic feature (e.g. increased tendency to metastasize, higher response to a chemotherapeutic agent, lengthened existence). Cancers are not just masses of malignant cells but complex ‘rogue’ organs, to which many other cells are recruited and can be degraded by the transformed cells. Interactions between malignant and non-transformed cells create the Tumor microenvironment (TME).
Track 4: Immunotherapy tumors
The mainstay of cancer treatment has historically involved therapies, such as surgery, chemotherapy or radiation that were developed without regard for the patient's immune system. These therapies include nonspecific activation of the immune system using tollâ€like receptor ligands, cytokines or immune checkpoint inhibitors, or specific treatments, like monoclonal antibody administration or vaccination, that directly target cancer cells. Perhaps, the most promising specific therapy is the adoptive transfer of genetically engineered tumourâ€reactive T cells, an approach that has already proven curative in some patients with metastatic disease. Cumulatively, these new immuneâ€based approaches have great promise to revolutionise cancer therapy.
Track 5: Tumor Immunogenicity
The Tumor microenvironment is an important aspect of cancer biology that contributes to Tumor initiation, Tumor progression and responses to therapy. Cells and molecules of the immune system are a fundamental component of the Tumor microenvironment. The ongoing battle between hosts and pathogens has long been of interest to evolutionary biologists. Because hosts and pathogens act as environments for each other, their intertwined struggle for existence is both continual and rapid. It is therefore little wonder that the host and pathogen genes that control infection and immunity frequently show high levels of genetic diversity and presents some of the best examples of positive selection (adaptive evolution) there are two main classifications of tumors. One is known as benign and the other as malignant. A benign Tumor is a Tumor that does not invade its surrounding tissue or spread around the body. A malignant Tumor is a Tumor that may invade its surrounding tissue or spread around the body.
Track 6: Cancer Vaccines
Most of us know about vaccines given to healthy people to help prevent infections, such as measles and chicken pox. These vaccines use weakened or killed germs like viruses or bacteria to start an immune response in the body. Getting the immune system ready to defend against these germs helps keep people from getting infections. Most cancer vaccines work the same way, but they make the person’s immune system attack cancer cells. The goal is to help treat cancer or to help keep it from coming back after other treatments. But there are also some vaccines that may actually help prevent certain cancers. Cancer treatment vaccines are different from the vaccines that work against viruses. These vaccines try to get the immune system to mount an attack against cancer cells in the body. Instead of preventing disease, they are meant to get the immune system to attack a disease that already exists. Some cancer treatment vaccines are made up of cancer cells, parts of cells, or pure antigens. Sometimes a patient’s own immune cells are removed and exposed to these substances in the lab to create the vaccine. Once the vaccine is ready, it’s injected into the body to increase the immune response against cancer cells. Vaccines are often combined with other substances or cells called adjuvants that help boost the immune response even further.
Track 7: Antibody Therapy of Cancer
Antibody marks the cancer cell and makes it easier for the immune system to find. The monoclonal antibody drug rituximab (Rituxan) attaches to a specific protein (CD20) found only on B cells, one type of white blood cell. Certain types of lymphomas arise from these same B cells. monoclonal antibodies can also function by attenuating hyperactive growth signals neo angiogenesis. A monoclonal antibody can be conjugated to a radioactive particle that will ensure directed delivery to the cancer cell and slow and long release of the radiation, hence maximizing chances of positive outcome and minimizing non-specific damaging exposure to radiation.
Track 8: Cancer Immunology & Immunotherapy
Immunotherapy is treatment that uses certain parts of a person’s immune system to fight diseases such as cancer. This can be done in a couple of ways: Own immune system stimulation, Biological therapy or biotherapy. These advances in cancer immunotherapy are the result of long-term investments in basic research on the immune system—research that continues today. Additional research is currently under way to: understand why immunotherapy is effective in some patients but not in other’s who have the same cancer, expand the use of immunotherapy to more types of cancer, increase the effectiveness of immunotherapy by combining it with other types of cancer treatment, such as targeted therapy, chemotherapy, and radiation therapy.
Track 9: Immune Checkpoint inhibitors
Immunology-based therapy is rapidly developing into an effective treatment option for a surprising range of cancers. We have learned over the last decade that powerful immunologic effector cells may be blocked by inhibitory regulatory pathways controlled by specific molecules often called "immune checkpoints." The development of a new therapeutic class of drugs that inhibit these inhibitory pathways has recently emerged as a potent strategy in oncology. Three sets of agents have emerged in clinical trials exploiting this strategy. These agents are antibody-based therapies targeting cytotoxic T-lymphocyte antigen 4 (CTLA4), programmed cell death 1 (PD-1), and programmed cell death ligand 1 (PD-L1). These inhibitors of immune inhibition have demonstrated extensive activity as single agents and in combinations. Clinical responses have been seen in melanoma, renal cell carcinoma, small cell lung cancer, and several other tumor types.
Track 10: Cancer Research
The goal of the Cancer Research Program is to make significant improvements in the prevention, early detection, diagnosis and treatment of cancer. It will continue to translate basic research findings into clinical applications together with strategic partners, with the National Centre for Tumor Diseases (NCT) and the nationally active German Consortium for Translational Cancer Research (DKTK) playing key roles. The program is also developing new approaches in the fields of cancer genome and epigenome research, metabolic dysfunction, personalized radiation oncology and ion therapy, molecular imaging, neuro-oncology, individualized cancer medicine and health economics.
Track 11: Combining Cancer Immunotherapies
Targeted therapies act by blocking essential biochemical pathways or mutant proteins that are required for tumor cell growth and survival. These drugs can arrest tumor progression and induce striking regressions in molecularly defined subsets of patients. Indeed, the first small molecule targeted agent, the BCR-ABL kinase inhibitor imatinib, rapidly induced complete cytogenetic responses in 76% of chronic myelogenous leukemia patients. Further research into the underlying genetic pathways driving tumor proliferation uncovered additional oncoproteins that are critical for tumor maintenance, such as the epidermal growth factor receptor (EGFR), BRAF, KIT, HER (also known as neu and ERBB) and anaplastic lymphoma kinase (ALK). Similar to imatinib, small molecule inhibitors of these kinases have effectuated impressive tumor responses in selected patients, although regressions are commonly followed by the development of progressive disease due to the emergence of drug-resistant variants. Resistance usually involves secondary mutations within the targeted protein or compensatory changes within the targeted pathway that bypass the drug-mediated inhibition. Accordingly, targeted therapies may elicit dramatic tumor regressions, but persistence is generally short-lived, limiting the overall clinical benefit.
Track 12: Tumor immunotherapy research
Immunotherapy is an innovative treatment approach that empowers the human immune system to overcome cancer and other debilitating diseases. The T-cell therapies are the most radical of several new approaches that recruit the immune system to attack cancers. The treatments work by removing molecular brakes that normally keep the body’s T cells from seeing cancer as an enemy, and they have helped demonstrate that the immune system is capable of destroying cancer. Immunotherapy may help boost the body’s immune response. This approach uses drugs/agents to trigger or stimulate the immune system to react to the invader – in this case, the cancer cells. This is similar to how a cold virus would stimulate your immune system.
Track 13: Cancer Micro and Immuno environment
Interactions between malignant and non-transformed cells create the Tumor microenvironment (TME). The non-malignant cells of the TME have a dynamic and often tumor-promoting function at all stages of carcinogenesis .Intercellular communication is driven by a complex and dynamic network of cytokines, chemokine’s, growth factors, and inflammatory and matrix remodeling enzymes against a background of major perturbations to the physical and chemical properties of the tissue. The evolution, structure and activities of the cells in the TME have many parallels with the processes of wound healing and inflammation, but cells such as macrophages are also found in cancers that have no known association with chronic inflammatory conditions.
Track 14: Tumor markers and drug targeting
Tumor markers are substances that are produced by cancer or by other cells of the body in response to cancer or certain benign (noncancerous) conditions. Most tumor markers are made by normal cells as well as by cancer cells; however, they are produced at much higher levels in cancerous conditions. These substances can be found in the blood, urine, stool, tumor tissue, or other tissues or bodily fluids of some patients with cancer. Most tumor markers are proteins. Thus far, more than 20 different tumor markers have been characterized and are in clinical use. Some are associated with only one type of cancer, whereas others are associated with two or more cancer types. There is no “universal” tumor marker that can detect any type of cancer. Among various approaches to specifically target drug-loaded carrier systems to required pathological sites in the body, two seem to be most advanced – passive (EPR effect-mediated) targeting, based on the longevity of the pharmaceutical carrier in the blood and its accumulation in pathological sites with compromised vasculature, and active targeting, based on the attachment of specific ligands to the surface of pharmaceutical carriers to recognize and bind pathological cells.
Track 15: Tumorigenesis
Tumorigenesis focuses on the multistep process of tumor Development, the critical progression of which is dependent on sequential accumulation of mutations within tissue cells, only a relatively small subset of which is crucial for malignant transformation, driven by the well-known pathways of tumorigenesis (growth signal self-sufficiency; anti-growth signal insensitivity; apoptosis evasion; unbound replicative potential; sustained angiogenesis; and tissue invasion and [potential metastasis). Tumorigenesis depends on carcinogenesis, but not vice versa, and when we focus on carcinogenesis, our scope rests predominantly with mutation or epimutation acquisition, while when we focus on tumorigenesis, our scope is on the multistep progress of mutated cells in tumor development.
Track 16: Cancer Clinical Trials
To developing new methods to prevent, detect, and treat cancer. It is through clinical trials that researchers can determine whether new treatments are safe and effective and work better than current treatments. Cancer clinical trials have led to scientific advances that have increased doctors' understanding of how and why tumor’s develop and grow. This knowledge has helped doctors make progress in preventing cancer, diagnosing cancer, slowing or stopping the development of cancer, and finding cancers that have come back after treatment.
Track 17: Tumor biology
Cancer cells behave as independent cells, growing without control to form tumors. Tumors grow in a series of steps. The first step is hyperplasia, meaning that there are too many cells resulting from uncontrolled cell division. These cells appear normal, but changes have occurred that result in some loss of control of growth. The second step is dysplasia, resulting from further growth, accompanied by abnormal changes to the cells. The third step requires additional changes, which result in cells that are even more abnormal and can now spread over a wider area of tissue. These cells begin to lose their original function; such cells are called anaplastic. At this stage, because the tumor is still contained within its original location (called in situ) and is not invasive, it is not considered malignant - it is potentially malignant. The last step occurs when the cells in the tumor metastasize, which means that they can invade surrounding tissue, including the bloodstream, and spread to other locations. This is the most serious type of tumor, but not all tumors progress to this point. Non-invasive tumors are said to be benign. The discovery of tumor stem cells in a range of cancers has created opportunities for researchers to identify these rare cells in both solid tumors and hematologic cancers, as well as to investigate the role of these cells at different stages of disease.The recognition that the cancer cell is in a symbiotic relationship with the tumor microenvironment has created opportunities to study the interactions of cancer cells within the tumor or the host microenvironment.
Track 18: Cancer Biomarkers
In cancer research and medicine, biomarkers are used in three primary ways:
- To help diagnose conditions, as in the case of identifying early stage cancers (Diagnostic)
- To forecast how aggressive a condition is, as in the case of determining a patient's ability to fare in the absence of treatment (Prognostic)
- To predict how well a patient will respond to treatment (Predictive)
Track 19: Immuno-Oncology studies
The immune system is the body’s natural defence system. It is a collection of organs, cells and special molecules that helps protect you from infections, cancer and other diseases. Immuno-oncology therapies activate our immune system, making it able to recognise cancer cells and destroy them. Breast cancer is one of the major cancer types for which new immune-based cancer treatments are currently in development. Lung cancer surgery carries risks, including bleeding and infection. Clinical trials are studies of experimental lung cancer treatments. Adult central nervous system tumor is a disease in which abnormal cells form in the tissues of the brain and/or spinal cord. A tumor that starts in another part of the body and spreads to the brain is called a metastatic brain tumor. There are different types of brain and spinal cord tumors such as Astrocytic Tumors, Oligodendroglial Tumors, Mixed Gliomas, Ependymal Tumors, Medulloblastomas, Pineal Parenchymal Tumors, Meningeal Tumors, Germ Cell Tumors, Craniopharyngiom. Advances in Immuno-oncology have given oncologists and their patients reason to be encouraged—the launch of immune checkpoint inhibitors and development of other immunotherapy assets for the treatment of several difficult-to-treat diseases, including metastatic melanoma and non-small cell lung cancer, represents great progress.
Track 20: Immunotherapy Monitoring
The development of methods to propagate immune T-cells, and in particular tumor specific T-cells from the patients with cancer, lead to an important breakthrough; the identification of MAGE-1,a melanoma-specific antigen that stimulates human T-cells in-vitro. With antigen specific T-cells as a reagents, it was possible to clone the MAGE-1 studies showed that the human immune system can respond tumor antigens, and the findings stimulated a productive effort to discover tumor antigens. The result is a long and still-growing list of antigens from a variety of tumor that could serve a variety of tumor’s that could serve as targets for treatment.
Track 21: Engineered T-Cell Therapy
Engineered T cells are the result of turning a therapeutic process into a product capable of overcoming checkpoint inhibition, and are the future of adoptive immunotherapy. Cytokine release syndrome,” a storm of molecules generated as the cells fights the cancer. Instead of an antibody, single-chain target domain, he used a human cytokine, IL-13, with a mutation in the sequence that gave high affinity for IL-13 receptor α2. These cells were infused intra cranially, establishing the safety of intracranial administration with some antitumor responses.
Track 22: Novel Approaches in Cancer & Tumor
Immunotherapy encompasses several different treatment approaches, each of which has a distinct mechanism of action, and all of which are designed to boost or restore immune function in some manner. This includes: Monoclonal antibodies, Immune checkpoint inhibitors, Therapeutic Cancer vaccines, cytokines, and other non-specific immunotherapies.
With the enormous response from the previous annual Tumor & Cancer Immunology conference 2016, ConferenceSeries LLC Ltd invites all the participants from all over the world to attend 2nd International Conference on Tumor & Cancer Immunology-2017” during July 17-18, 2017 in Chicago, USA which includes prompt keynote presentations, Oral talks, Poster presentations and Exhibitions. The Tumor & Cancer Immunology Conference hosting presentations from editors of prominent refereed journals, renowned and active investigators and decision makers in the field of Immunology.
Tumor & Cancer Immunology -2017 Conference deals with the diagnosis, prevention, and treatment of diseases of the organ specific cancers and including the latest techniques. Tumor & Cancer Immunology 2017 is an extraordinary event designed for International medical health professionals and oncologists to facilitate the dissemination and application of research findings related to Cancer. Head and Neck Cancer The conference invites participants from all leading universities, clinical research institutions and diagnostic companies to share their research experiences on all aspects of this rapidly expanding field and thereby, providing a showcase of the latest techniques. Tumor & Cancer Immunology 2017 provides three days of robust discussions on methods and strategies related to management and quality improvement of Cancer therapy, Tumor Biomarkers as well as explore new ideas and concepts on a global scale and the topics include breast cancer, leukaemia, bone cancer, lung cancer, prostate cancer, thyroid cancer, blood cancer, colon cancer and cervical cancer.
Why to attend??
With members from around the world focused on learning about Tumor or Cancer immunology and its advances: this is your best opportunity to reach the largest assemblage of participants from Tumor & Cancer immunology community. conduct presentations, distribute information’s, meet with current and potential scientists, make a splash with new drug developments, and receive name recognition at this 2-day event, world-renowned speakers, the most recent techniques, developments, and the newest updates in Tumor & Cancer immunology are hallmarks of this conference.
Target Audience
- Tumor & Cancer research Students, Scientists
- Tumor & Cancer Researchers
- Tumor & Cancer research Faculty
- Oncologist
- Medical Colleges
- Tumor or Cancer research Associations and Societies
- Business Entrepreneurs
- Training Institutes
- Manufacturing Medical Devices Companies
Join us in Chicago, USA for the leading annual Tumor & Cancer immunology 2017 event and
Find the latest developments in immunology and immunotherapy
Lectures by the world's prominent Tumor Researchers, oncologist and poster presentations at every career stage.
Network Tumor immunology and Immunotherapy with colleagues from more than 50 countries
Awareness on novel tools and techniques to benefit your research.
2nd International Conference on Tumor & Cancer Immunology and Immunotherapy to be held during July 17-18, 2017 Chicago, USA with the theme of “Emerging Technologies and treatment in Tumor & Cancer immunotherapy from vaccines to antibodies and cell therapies”
Scope of Tumor & Cancer immunology:
In most individuals the immune system recognizes and eliminates Tumor cells. However Tumor may overcome immunosurveillance using a broad repertoire of subversive tactics. In this research theme, through investigation of the normal and compromised immune system, we explore the mechanisms by which the Tumor cell may tip the balance between immune control and immune evasion. The pace of change in cancer care is accelerating. A cluster of innovative treatments, often combined with other new or existing medicines, and frequently associated with biomarkers, are emerging from the research and development pipeline.
Tumor Immunotherapy Market Value Report Highlights
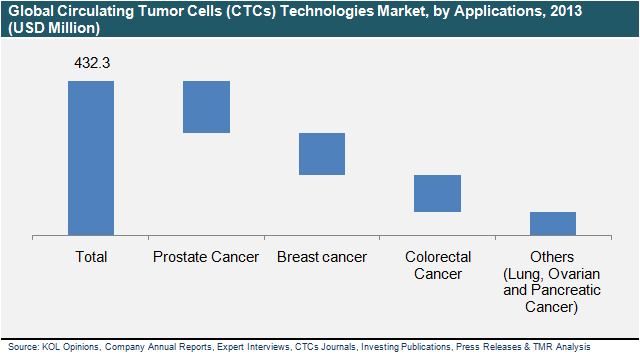
This report provides the market analysis for various technologies and applications used for the enrichment and detection of circulating tumor cells (CTCs). Based on tumor cell detection technologies, the market is segmented into molecular methods and optical methods. Furthermore, based on the applications, the CTC prognostic technologies market is segmented into breast cancer, colorectal cancer, prostate cancer and others (lung, ovarian and pancreatic cancer). Market forecast for all these segments has been provided in the report for the period 2012 to 2020 in terms of USD million, along with CAGR for the forecast period 2014 to 2020, considering 2013 as the base year.
Global circulating Tumor cells market, by technology, 2012 – 2020 (USD Million)

Tumor cell enrichment products and Tumor cell detection are two technologies analysed in this study. In the forecast period, Tumor cell enrichment technology is expected to grow at a CAGR of 26.1%. Immunological and immunomagnetic technology of cell enrichment technology is expected to have highest CAGR in the forecast period due to effective analysis with comparatively less blood sample (20 ml blood analysed in 30 min) and its usability with whole genome sequencing. Research and development in the field of biomarker assessment is additionally expected to boost the growth of circulating Tumor cells market in the next six years.
Cancer Immunotherapy Market Value Report Highlights
The world spent an all-time high of $100 billion on cancer medicines in 2014, up 33 percent from $75 billion just five years ago. Overall, global spending on cancer drugs has risen at an annual rate of 6.5 percent for the past five years, but jumped 10.3 percent in 2014, a new report by the IMS Institute for Healthcare Informatics states.
The spending is concentrated in only a handful of nations. The U.S. and the five largest European countries -- Britain, France, Germany, Italy and Spain -- make up two-thirds of global spending on these medicines. The U.S. spent $42.5 billion on cancer drugs in 2014, which accounted for 11.3 percent of the nation’s total spending on all drugs. The "pharmerging" group of countries (see graph below) represents 17 nations that IMS has identified as likely to represent 50 percent of global growth in pharmaceutical sales over a five-year period through 2017.
The report also shows that American patients are bearing the brunt of higher prices. The average cost of all treatments that a cancer patient undergoes over the course of a month has risen by 39 percent in the past 10 years. Though a portion of their bill may be covered by insurers, Americans still saw a 71 percent increase in out-of-pocket costs for intravenous drugs in just one year, from 2012 to 2013.
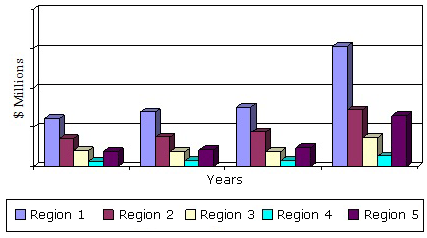
The global cancer immunotherapies market reached $30.8 billion in 2012. This market is expected to grow to nearly $34.3 billion in 2013 and $67.9 billion in 2018 with a compound annual growth rate (CAGR) of 14.7% over the five-year period, 2013 to 2018.
This report provides:
· An overview of the global market for cancer immunotherapies
· Analyses of global market trends, with data from 2012, estimates for 2013, and projections of CAGRs through 2018.
· Analyses of factors influencing market demand such as clinical guidelines, demographic changes, and market saturation
· Technological discussion including the current state, newly issued patents, and pending applications
· Profiles of leading companies in the industry.
Target Audience
- Tumor & Cancer Research Students, Scientists
- Tumor & Cancer Researchers
- Tumor & Cancer Immunology Faculty
- Oncologist, Young Researchers
- Medical Colleges
- Physicians/Consultants
- Geneticist
- Immunology Associations and Societies
- Business Entrepreneurs
- Training Institutes
- Manufacturing Medical Devices Companies
Why to attend?
- Best platform to develop new partnership & collaborations.
- Best location to speed up your route into every territory in the World.
- 89% our conference attendees are the Key contact in their labs purchasing decisions.
- Our exhibitor booths were visited 4-5 times by 80% of the attendees during the conference.
- Past exhibitor’s feedback reveals ample of enquiries perceived from the conference attendees.
- Network development with both Academia and Business.
Why Chicago?
Chicago is the third most populous city in the United States. It is the most populous city in the state of Illinois and the Midwest with over 2.7 million residents. The Chicago metropolitan area is home to nearly 10 million people and is the third-largest in the United States. Chicago is the seat of Cook County.
Chicago was incorporated as a city in 1837, near a portage between the Great Lakes and the Mississippi River watershed, and experienced rapid growth in the mid-nineteenth century. Today, the city is an international hub for finance, commerce, industry, technology, telecommunications, and transportation, with O'Hare International Airport being the busiest airport in the world; it also has the largest number of U.S. highways and railroad freight. In 2012, Chicago was listed as an alpha global city by the Globalization and World Cities Research Network, and ranks seventh in the world in the 2014 Global Cities Index. As of 2012, Chicago had the third largest gross metropolitan product in the United States at US$571billion. Apart from this Chicago is home to several scientists and professors from several fields and this makes it ideal place for the conference.
Conference Highlights
- Antibody Therapy of Cancer
- Tumor Immunogenicity
- Tumors
- Brain Tumors
- Immunotherapy - Tumors
- Tumor Immunology
- Cancer vaccines
- Cancer Immunology & Immunotherapy
- Immune checkpoint inhibitors
- Cancer Research
- Combining Cancer Immunotherapies
- Tumor immunotherapy research
- Cancer micro and immuno environment
- Tumor markers and drug targeting
- Tumorigenesis
- Cancer clinical trials
- Tumor biology
- Cancer biomarkers
- Immuno-Oncology studies
- Immunotherapy Monitoring
- Engineered T-Cell Therapy
- Novel Approaches in Cancer & Tumor
To share your views and research, please click here to register for the Conference.
To Collaborate Scientific Professionals around the World
| Conference Date | July 17-18, 2017 | ||
| Sponsors & Exhibitors |
|
||
| Speaker Opportunity Closed | Day 1 | Day 2 | |
| Poster Opportunity Closed | Click Here to View | ||
Useful Links
Special Issues
All accepted abstracts will be published in respective Our International Journals.
Abstracts will be provided with Digital Object Identifier by

























